TEAM Launched January 2026
Your 2026 TEAM performance will determine your financial risk for the next four years.
CMS's mandatory bundled payment model is now live.
What your hospital does in 2026 sets the reinbursement baseline CMS uses when penalties begin in 2027.
NOW
2026
Upside only. No penalties.
Your benchmark is being set right now
RISK BEGINS
2027
Two sided risk starts
Your 2026 performance determines your target price
ACTIVE PENALTIES
2027-2030
Penalties and bonuses calculated against your locked baseline
Caregentic is a TEAM
episode operations layer
Not a chatbot. Not a portal. Not another point solution.

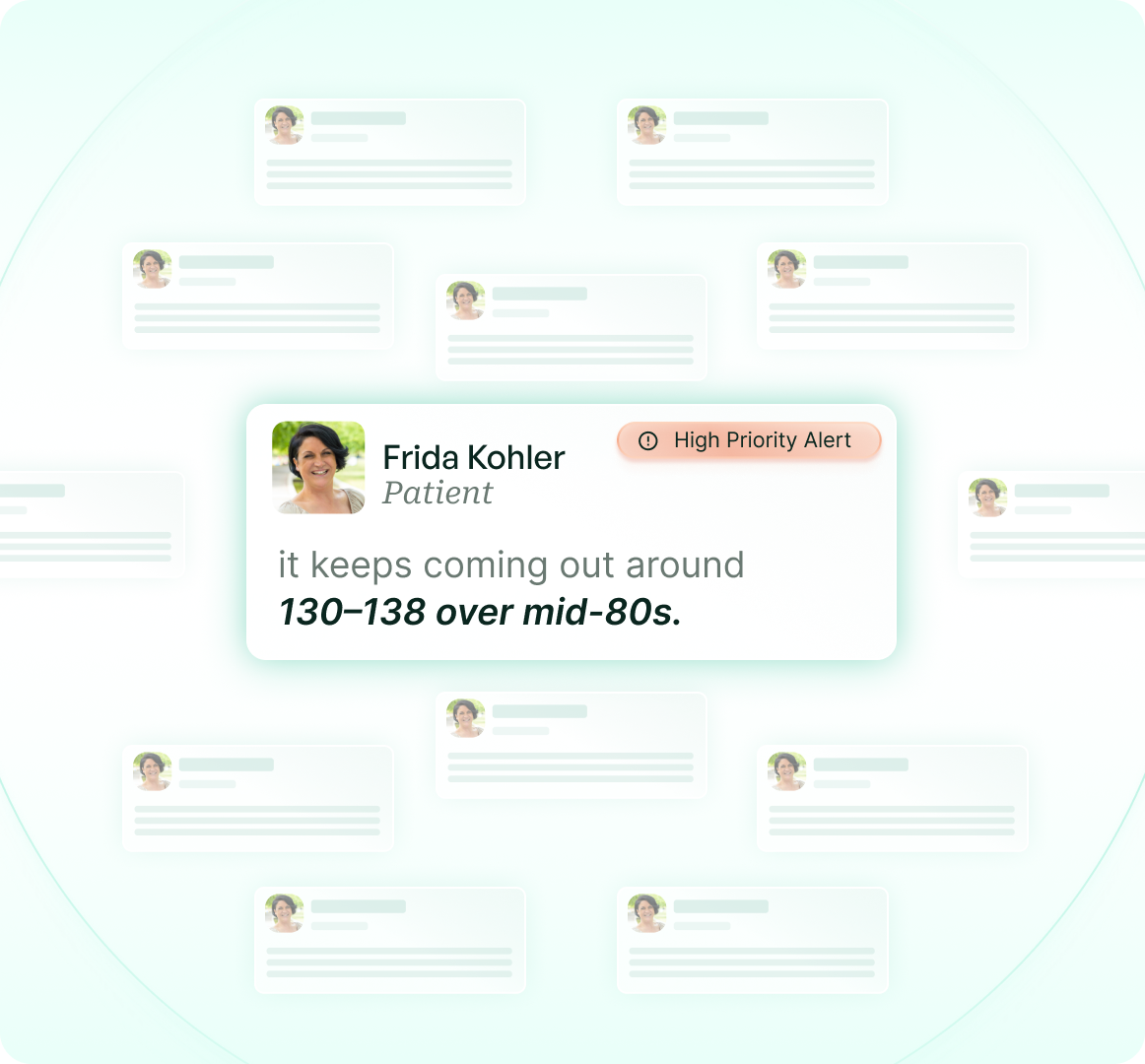
Automated 30-Day Patient Monitoring
Post-discharge education, reminders, check-ins, symptom tracking, and scheduling — all handled via SMS across the full episode window, without staff involvement.
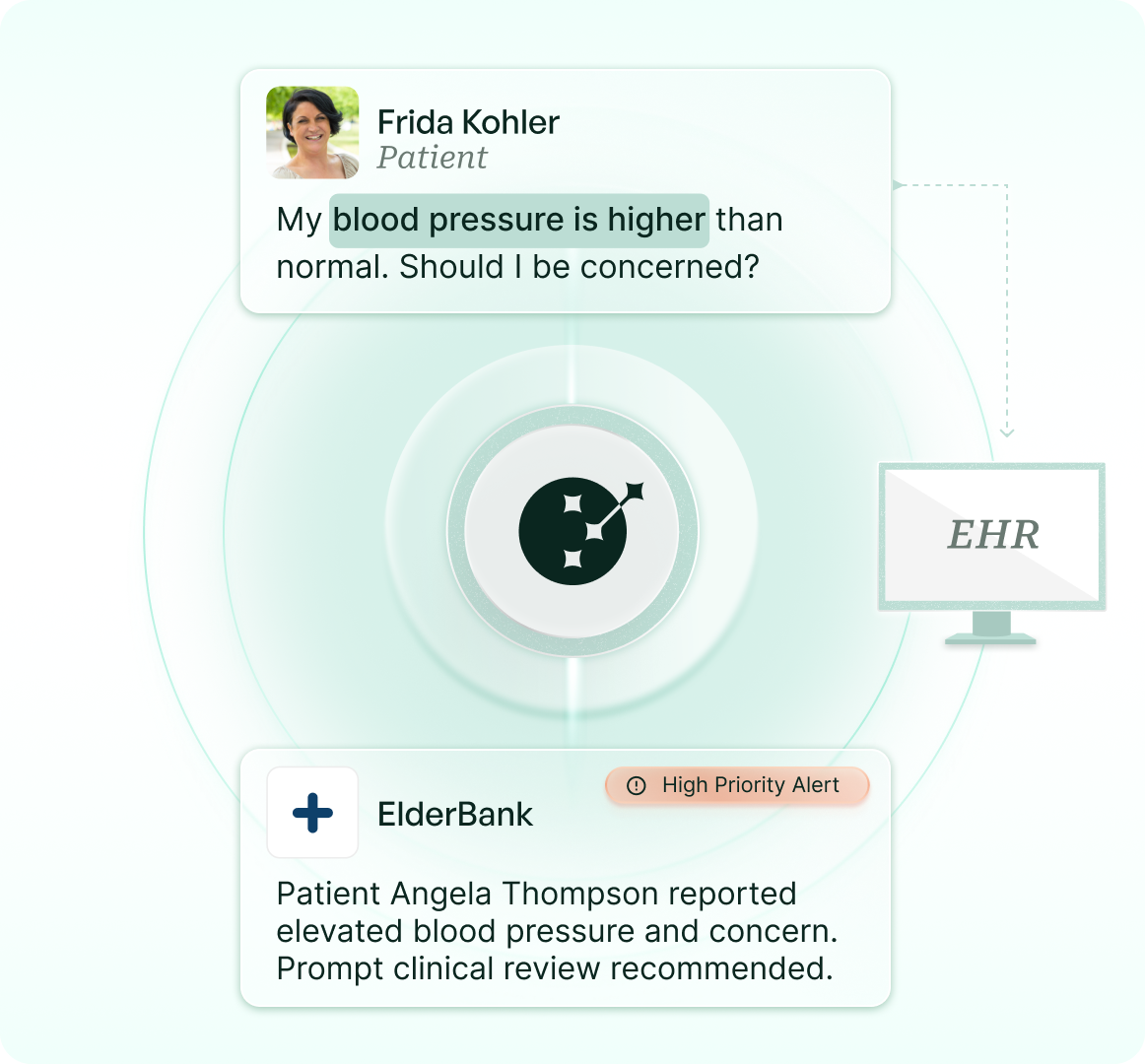
Intelligent Alert Routing
Post-discharge education, reminders, check-ins, symptom tracking, and scheduling — all handled via SMS across the full episode window, without staff involvement.
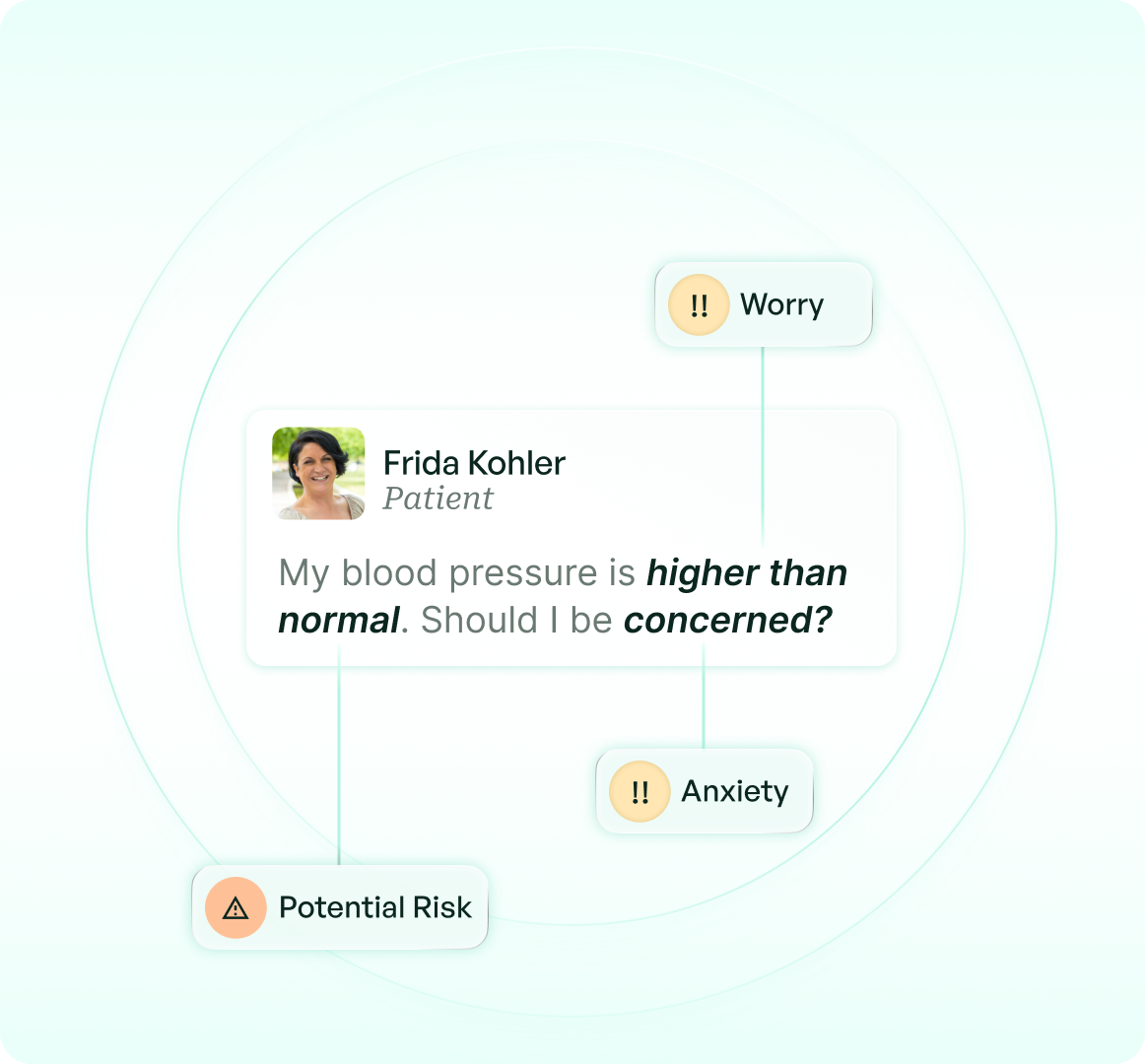
Structured Episode Intelligence
Post-discharge education, reminders, check-ins, symptom tracking, and scheduling — all handled via SMS across the full episode window, without staff involvement.
Automatic EHR Documentation
Post-discharge education, reminders, check-ins, symptom tracking, and scheduling — all handled via SMS across the full episode window, without staff involvement.

measurable IMPACT
63%
reduction in clinician time spent on EHR-related admin tasks
92%
Appointment show rate = fewer missed follow-ups that lead to complications
93NPS
NPS vs. 30–40 industry benchmark = engaged patients who follow discharge instructions
Results from previous Caregentic deployments with leading health systems.
Episode intelligence
for the 30-day post-discharge window
HIPAA Compliant
SOC 2 Type II
EHR Integration
90-Day Deployment
Ready to map your TEAM readiness?
Our CEO Russ Johannesson will walk through
what this means for your facility in 15 minutes.